GLP-1 Agonist Therapy for Pelvic Organ Prolapse: A Promising Solution?
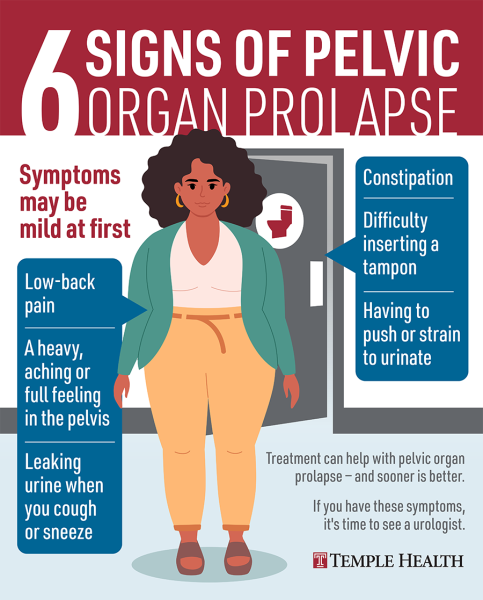
Pelvic organ prolapse (POP) is a common condition that affects millions of women worldwide, causing various symptoms such as pelvic pain, pressure, and bladder or bowel incontinence. While current treatment options for POP include lifestyle modifications, pelvic floor muscle training, pessaries, and surgery, researchers are exploring the potential benefits of glucagon-like peptide-1 (GLP-1) agonist therapy in addressing this condition.
GLP-1 Agonists: A Class of Medications for Weight Loss and Glycemic Control
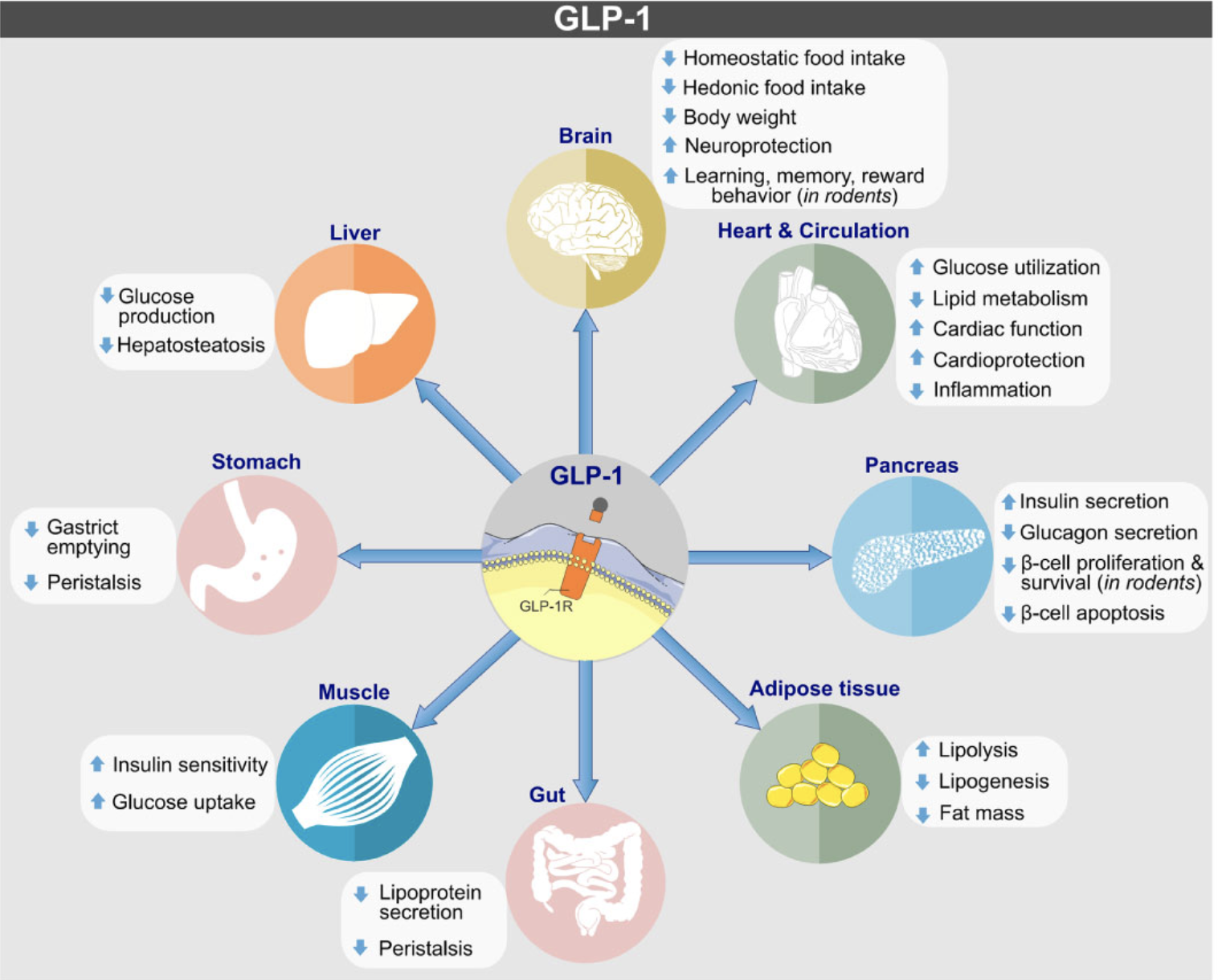
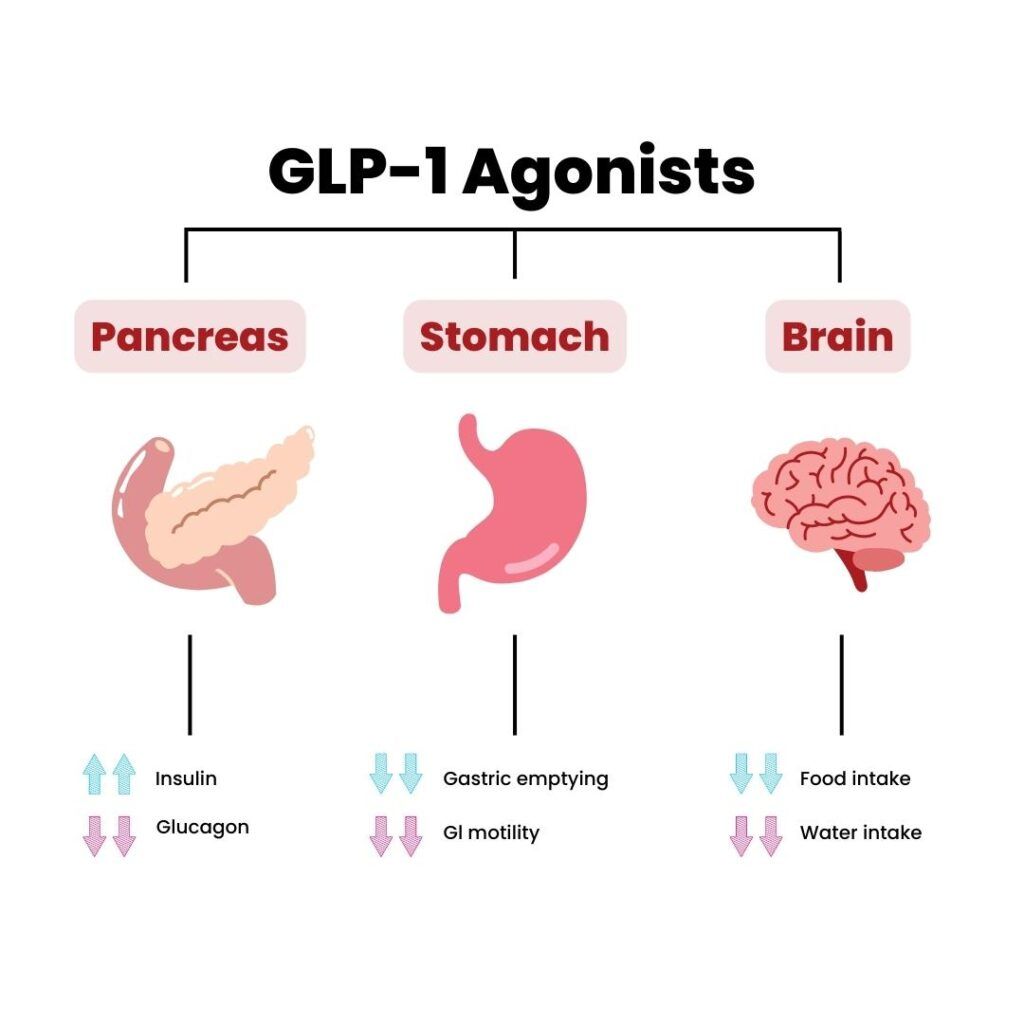
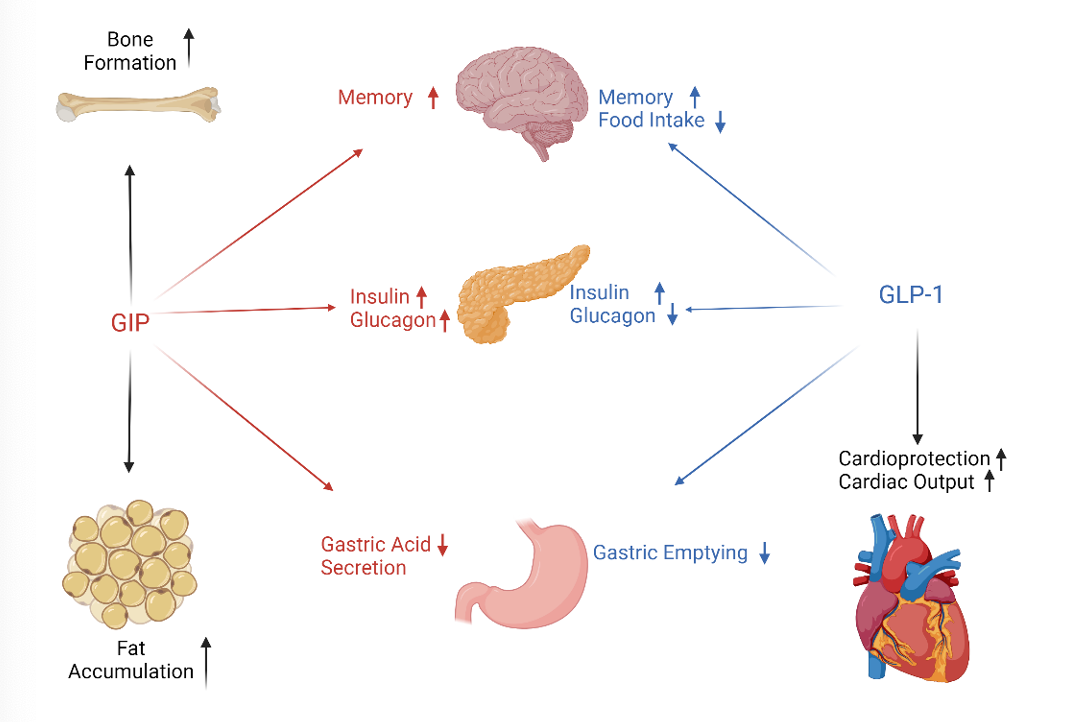
GLP-1 receptor agonists (GLP-1RAs) are a type of medication that mimic the action of the incretin hormone, GLP-1, which plays a crucial role in glucose homeostasis. These medications have gained popularity in recent years due to their ability to improve glycemic control and facilitate weight loss in individuals with type 2 diabetes and obesity.
The Connection Between GLP-1 Agonists and Pelvic Organ Prolapse
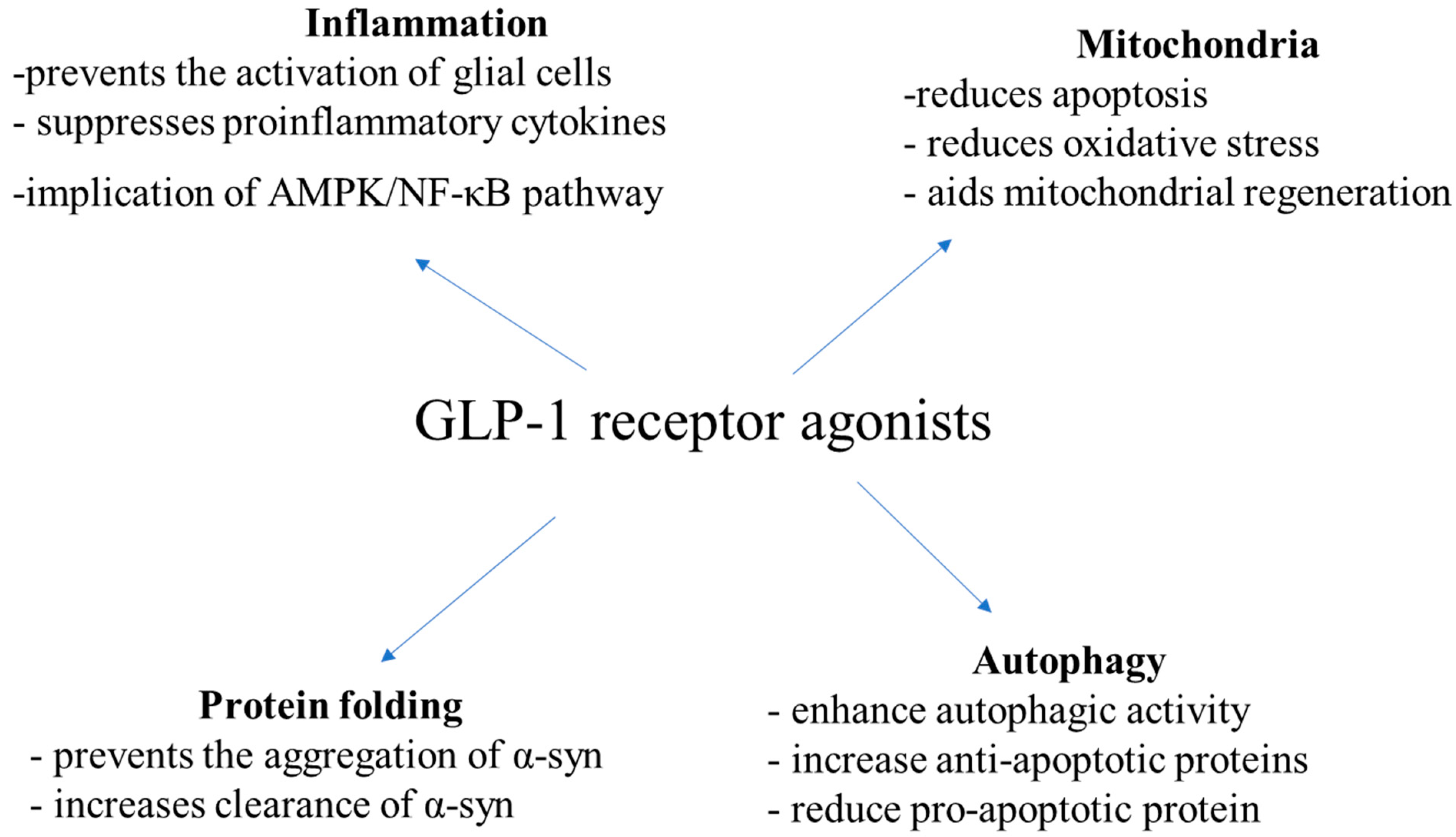
Recent studies suggest that GLP-1 agonists may have a positive impact on pelvic floor function and reduce the risk of pelvic organ prolapse. This is attributed to the medication's effects on weight loss, improved glycemic control, and the reduction of inflammation. Additionally, GLP-1RAs have been shown to stimulate the contraction of the pelvic floor muscles, which can help alleviate symptoms associated with POP.
Clinical Evidence Supporting GLP-1 Agonist Therapy for POP
Several clinical studies have investigated the effects of GLP-1 agonists on pelvic floor function and POP. A 2022 study published in the Journal of Clinical Endocrinology and Metabolism found that GLP-1RAs reduced the incidence of POP by 30% in women with type 2 diabetes. Another study published in the International Urogynecology Journal in 2023 found that GLP-1 agonist therapy significantly improved pelvic floor function and reduced symptoms associated with POP in women with obesity.
Benefits and Potential Risks of GLP-1 Agonist Therapy for POP
The potential benefits of GLP-1 agonist therapy for POP include improved glycemic control, weight loss, and reduced inflammation. However, as with any medication, there are potential risks to consider, including gastrointestinal adverse effects, hypersensitivity reactions, and the potential for medication resistance. It is essential to consult with a healthcare professional to discuss the potential benefits and risks of GLP-1 agonist therapy for POP.
Conclusion
GLP-1 agonist therapy for pelvic organ prolapse is a promising area of research that holds significant promise for women suffering from this condition. While current treatment options for POP exist, the potential benefits of GLP-1 agonist therapy, including improved glycemic control, weight loss, and reduced inflammation, make it an attractive adjunctive treatment option. Further research is needed to fully understand the effects of GLP-1RAs on POP and to establish optimal treatment protocols.